Beyond the Surgeon’s Hands: The Hidden Engineering That Makes Organ Transplants Possible
KAMPALA, UGANDA – When most people think of an organ transplant, they picture a surgeon’s steady hands and life-changing moment of connection. Joel Aita, CEO of Joadah Group, thinks of a building.
“Before a single suture is placed, an extraordinary engineering ecosystem must already be in perfect operation,” says Aita, whose company specialises in hospital infrastructure.
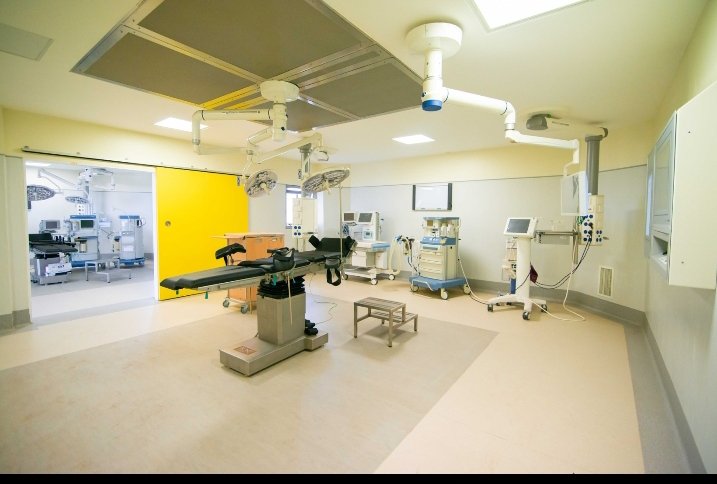
That ecosystem begins with the operating theatre itself—but not just any theatre. Transplant surgery demands what Aita describes as a “2-in-1 facility”: separate rooms for donor and recipient, connected by invisible engineering.
At the heart of this environment sits the laminar flow system, a precision air movement technology that delivers ultra-clean air in a single, unidirectional stream directly over the sterile field. The system cycles the entire room’s air up to 500 times per hour, creating a protective curtain of purity. The goal? Reduce airborne contamination to near zero.
“In transplant surgery, a single airborne pathogen can cost a life,” Aita explains.
The Piped Matrix
Behind theatre walls runs an extensive network of over ten piped medical gases—oxygen, nitrous oxide, medical air, carbon dioxide, nitrogen, helium, argon, xenon, vacuum systems, and medical vacuum suction. Each line features colour-coded pipelines, pressure regulators, zone valves, and alarm systems. Every system is engineered with 100% redundancy. Failure of any one mid-surgery is catastrophic.
Where the Journey Actually Begins
Perhaps the most surprising revelation comes when Aita describes where transplant truly starts: not in the operating theatre, but in a dedicated intensive care unit, sometimes a full week before surgery.
Why? The patient’s immune system must be deliberately suppressed—reduced almost to zero—before the new organ arrives. This prevents organ rejection, the body’s natural defence mechanism that attacks foreign tissue.
But this medical necessity creates an extraordinary engineering challenge. A patient with near-zero immunity is profoundly fragile. Their ICU environment must function as an external immune system.
That means positive pressure rooms where air flows outward to prevent pathogen entry, HEPA filtration capturing particles as small as 0.3 microns, dedicated nursing stations with full barrier protocols, and building management systems monitoring temperature, humidity, and air changes in real time.
Power and HVAC: The Unsung Heroes
The electrical infrastructure alone requires uninterruptible power supplies, standby generators with automatic transfer switches, Category 1 essential circuits that never go dark, and isolated power systems to prevent micro-shock to open-body patients.
The heating, ventilation and air conditioning system is its own discipline: operating theatres demand minimum 20 air changes per hour (25–30 for transplant), temperature control within ±0.5°C, and humidity held between 40 and 60 percent to prevent both static electricity and infection.
“If HVAC fails, surgery stops. Full stop,” Aita says.
The Bottom Line
“Organ transplantation is rightly celebrated as a triumph of medicine,” Aita concludes. “But it is equally a triumph of engineering. Every life saved on that table was first saved by an HVAC engineer who specified the laminar flow unit, an electrical engineer who designed the UPS system, a medical gas engineer who sized the pipeline manifolds.
“We do not wear scrubs. We do not stand at the table. But we built the table.”